An employee terms and you notify your COBRA administrator of the qualifying event. A letter goes out and you are done, right?
Well, yes and no.
It is important that a COBRA Qualifying Event Notice is:
(1) provided to required individuals and
(2) contains the appropriate details regarding COBRA coverage and election rights.
Who needs to receive a COBRA qualifying event notice?
In two words: Qualified beneficiaries.
Who counts as a qualified beneficiary?
A qualified beneficiary (QB) is a catch all term. Technically, a QB is anyone that experiences a qualifying event. For the purposes of this blog, we’ll confine the definition of QB to a covered employee, a covered employee’s spouse or a covered employee’s dependent.
When does a QB need to receive a COBRA qualifying event notice?
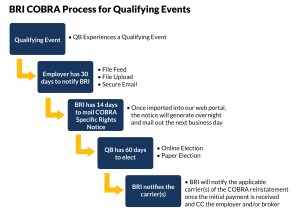
After a qualifying event occurs, you have 30 days to notify your COBRA administrator. Once your COBRA administrator is made aware that a qualifying event has occurred, they have 14 days to notify QBs about their right to elect COBRA coverage.
Overall, within 44 business days of the qualifying event, a QB must be sent a Specific Rights Notice.
Since QBs have independent election rights, they must each be notified. If all the QBs reside at the same address, the plan administrator has two options:
- Send separate election notices for each QB in a single mailing that is addressed to both the employee and spouse
- Send a single notice that clearly identifies all qualified beneficiaries covered by the notice
If the administrator chooses to send single notices, each one must explain each QB’s separate and independent right to elect COBRA continuation coverage.
After receiving the election notice, each QB has 60 days to decide if they want to elect continuation coverage.
What needs to be included in a COBRA qualifying event notice?
Quite a bit. There are just under a dozen items. (We’re not joking). They’re mostly dates, amounts, “how-to’s” and “you really ought to knows”.
The 11 items are:
- A written explanation of the procedures for electing COBRA
- The date by which the election must be made
- How to notify the plan administrator of the election
- The date COBRA coverage will begin
- The maximum period of continuation coverage
- The monthly premium amount
- The due date for the monthly payments
- Any applicable premium amount due for a retroactive period of coverage
- The address to which to send premium payments
- A qualified beneficiary’s rights and obligations with respect to extensions of COBRA coverage
- The basis for early termination of the period of COBRA coverage
As an employer, understanding these guidelines is essential to a compliant COBRA program. However, the qualifying notice is just the beginning.
Comprehensive COBRA administration service will incorporate procedures and reporting across proof of mail, premium collection, record retention and COBRA participant services.
Are you evaluating your COBRA administration services? Consider Benefit Resource.